
Key Takeaways
- Your oral microbiome directly influences cardiovascular health, diabetes management, and immune function—making preventative dental care a systemic health investment, not just cosmetic maintenance.
- Biofilm management (not just “brushing”) is the core of prevention: disrupting bacterial colonies before they produce the acids and toxins that cause decay, gum disease, and inflammation.
- The first 1,000 days of a child’s life establish lifelong oral immunity patterns, making early preventative care a generational health decision.
- Advanced diagnostic technology can now detect demineralization and disease at the cellular level—before pain, cavities, or bone loss occur—allowing truly minimally invasive intervention.
Why Your Mouth is the Gateway to Total Body Health
Most people think of dental appointments as separate from “real” healthcare. But here’s what the research shows: the bacteria living in your mouth don’t stay in your mouth.
When gum tissue becomes inflamed—even at levels you might not notice—it creates microscopic pathways for oral bacteria to enter your bloodstream. These bacteria trigger immune responses throughout your body. Studies published by the American Heart Association have identified specific oral pathogens in arterial plaque formations. The connection isn’t theoretical—it’s measurable.
For patients managing diabetes, the relationship runs both ways. Elevated blood sugar creates an ideal environment for harmful oral bacteria to thrive, while the inflammation from gum disease makes blood sugar harder to control. This creates a cycle where each condition worsens the other.
Pregnancy outcomes, respiratory infections, and even rheumatoid arthritis severity have documented links to oral health status. This isn’t about fear—it’s about understanding that your mouth is an integrated part of your body’s ecosystem, not an isolated system.
At Avra Dental in Ventura, we approach preventative care through this lens. When we’re removing calculus deposits or measuring periodontal pocket depths, we’re not just protecting your teeth. We’re managing inflammation that affects your entire body. That shift in perspective—from “dental hygiene” to “systemic health protocol”—changes how patients think about those six-month appointments.
The stakes are higher than avoiding a filling. Preventative dental care is cardiovascular care. It’s metabolic care. It’s immune system support. And it starts with understanding what you’re actually preventing.
The Science of Biofilm: Understanding What You’re Actually Preventing
Let’s talk about what’s really happening in your mouth between dental visits.
Biofilm is the technical term for what most people call “plaque,” but that word doesn’t capture what it actually is: a highly organized colony of bacteria living in a self-produced protective matrix. These aren’t random germs floating around. They’re communities with structure, communication systems, and survival strategies.
Within hours of your last cleaning, bacteria begin adhering to tooth surfaces. Within 24 hours, they’ve formed the early stages of biofilm. Within days, this film matures into a complex ecosystem where different bacterial species occupy specific niches—some thrive in oxygen-rich environments near the gumline, while others prefer the oxygen-depleted pockets below it.
Here’s why this matters: mature biofilm is up to 1,000 times more resistant to antimicrobials than individual bacteria. That’s why rinsing with mouthwash alone doesn’t work. The protective matrix shields the bacteria underneath from chemical disruption. Mechanical removal—through brushing, flossing, and professional instrumentation—is the only reliable way to break up these colonies before they cause damage.
The damage comes from bacterial metabolism. As these organisms consume sugars and starches from your diet, they produce acid as a waste product. When biofilm sits undisturbed on tooth enamel, these acids create localized pH drops. Enamel begins to demineralize when pH falls below 5.5. If this acid attack continues without intervention, demineralization progresses to cavitation—what we call a cavity.
Below the gumline, different bacteria dominate. Anaerobic species produce toxins that trigger your immune system to attack not just the bacteria, but your own gum tissue and bone. This is periodontal disease: your body destroying its own support structures in response to chronic bacterial presence. The inflammation is protective in intent but destructive in outcome.
Understanding biofilm as an organized threat—not just “dirty teeth”—reframes what preventative care actually does. You’re not just making your smile prettier. You’re systematically disrupting bacterial colonies before they can produce the acids and toxins that cause disease. That’s biofilm management. That’s the protocol.
At our Ventura dental office, we use advanced diagnostic tools to detect biofilm accumulation in areas you might miss at home. We’re looking for early warning signs: bleeding on probing, pocket depth increases, and areas of demineralization visible on digital radiographs. These indicators tell us where biofilm is winning, so we can intervene before irreversible damage occurs.
The Preventative Care Protocol: Professional Services That Stop Disease Before It Starts
Professional preventative care isn’t about “getting your teeth cleaned.” It’s a diagnostic and therapeutic protocol designed to detect and interrupt disease processes at their earliest, most reversible stages.
Comprehensive Examination: The Diagnostic Foundation
Every preventative visit at Avra Dental begins with a thorough clinical examination. We’re assessing tooth structure, gum tissue architecture, occlusion (bite alignment), oral mucosa, and temporomandibular joint function. We document pocket depths around each tooth, noting any increases from previous visits—a key indicator of active periodontal disease.
Digital radiography allows us to see what clinical examination cannot: interproximal decay (between teeth), bone levels, root structure, developing abscesses, and even early signs of oral pathology. These images use up to 90% less radiation than traditional film X-rays while providing higher resolution. We can detect demineralization before it becomes a cavity, giving us the option to attempt remineralization through fluoride therapy rather than immediately moving to restoration.
Intraoral cameras capture detailed images of individual teeth and gum tissue, allowing both our team and our patients to see exactly what we’re seeing. This visual documentation is powerful—when you can see the hairline crack in your molar or the inflammation around a filling margin, the need for intervention becomes clear.
Professional Prophylaxis: Disrupting Biofilm Where Home Care Cannot Reach
Even with excellent home care, calculus (hardened biofilm) forms in areas difficult to access—behind lower front teeth, around back molars, and below the gumline. Once biofilm mineralizes into calculus, it cannot be removed by brushing or flossing. It requires professional instrumentation.
Our dental hygienists use specialized scalers and ultrasonic instruments to remove these deposits. Ultrasonic scalers use high-frequency vibrations to break up calculus while simultaneously irrigating the area, flushing out bacteria and debris. Hand scaling allows for tactile precision in areas where calculus is tenacious or where tissue is sensitive.
This isn’t “just a cleaning.” It’s the mechanical disruption of mature biofilm communities and the removal of mineralized deposits that serve as anchoring points for new bacterial colonization. Without this professional intervention, even diligent home care cannot fully control biofilm accumulation.

Fluoride Therapy: Remineralization and Enamel Strengthening
Fluoride works through a chemical process called remineralization. When applied to tooth enamel, fluoride ions integrate into the crystal structure, creating fluorapatite—a compound more resistant to acid attack than the original hydroxyapatite. This isn’t coating the tooth; it’s chemically altering the enamel at a molecular level.
For patients with high caries risk—whether due to diet, medication-induced dry mouth, or genetic factors—professional fluoride applications provide a concentrated dose that significantly exceeds what’s available in over-the-counter products. We’re giving your enamel chemical reinforcement against the acid attacks it faces daily.
Sealants: Physical Barriers in High-Risk Areas
Molar teeth have deep grooves and pits that trap food particles and bacteria. Even with proper brushing, these fissures are difficult to clean completely. Dental sealants are thin, protective coatings applied to these chewing surfaces, effectively “sealing out” bacteria and food debris.
While most commonly applied to children’s permanent molars as they erupt, adults with deep grooves and no existing decay in those teeth can also benefit. The application is quick, non-invasive, and can prevent decay for years. This is truly preventative—stopping disease before it starts rather than treating damage after it occurs.
Periodontal Maintenance: Managing Chronic Inflammation
For patients with a history of periodontal disease, standard prophylaxis isn’t sufficient. Periodontal maintenance involves more frequent visits (typically every 3-4 months) and more intensive cleaning below the gumline to manage the chronic bacterial challenge. This isn’t “extra” care—it’s the minimum required to prevent disease recurrence in patients whose oral ecosystems are predisposed to pathogenic bacterial overgrowth.
We measure and document pocket depths at each visit, looking for stability or improvement. Bleeding on probing, increasing pocket depths, or bone loss visible on radiographs indicate that the current protocol isn’t controlling the bacterial challenge, and we adjust accordingly—whether through more frequent visits, adjunctive antimicrobial therapy, or referral to a periodontal specialist.
This is early intervention in action: catching inflammation before attachment loss, catching demineralization before cavitation, catching disease before pain. By the time a dental problem hurts, significant damage has already occurred. Professional preventative care operates in that window before symptoms appear—when intervention is simplest, least invasive, and most effective.
Your Daily Biofilm Management Routine
Professional care every six months isn’t enough on its own. Daily biofilm disruption at home is the foundation that makes professional intervention effective.
The Mechanics of Effective Brushing
Brush twice daily for two minutes using a soft-bristled brush and fluoride toothpaste. The technique matters more than the tool. Hold your brush at a 45-degree angle to your gumline—this positions the bristles to clean both the tooth surface and the sulcus (the shallow groove where tooth meets gum). Use gentle, circular motions rather than aggressive back-and-forth scrubbing, which can damage enamel and cause gum recession.
Many patients benefit from electric toothbrushes, which provide consistent motion and often include timers to ensure adequate brushing duration. The key is thoroughness: every tooth surface, including the backs of your back molars and the inside surfaces of your front teeth.
Replace your toothbrush or brush head every three months, or sooner if bristles become frayed. Worn bristles lose effectiveness and can harbor bacteria.
Interdental Cleaning: The Non-Negotiable Step
Brushing cleans only about 60% of tooth surfaces. The other 40%—the areas between teeth—require interdental cleaning. Dental floss remains the gold standard. Curve the floss around each tooth in a C-shape and move it gently up and down, going slightly below the gumline to disrupt biofilm in the sulcus.
If traditional flossing is challenging due to dexterity issues, tight contacts, or dental work, alternatives exist. Water flossers use pulsating water streams to flush out debris and biofilm. Interdental brushes—small, cone-shaped brushes—can clean between teeth when space allows. The best interdental cleaning method is the one you’ll actually use consistently.
Antimicrobial Rinses: Supplemental, Not Substitute
Antimicrobial mouthwashes can reduce bacterial counts and freshen breath, but they cannot replace mechanical cleaning. Remember: mature biofilm’s protective matrix shields bacteria from chemical agents. Rinses work best as supplements to brushing and flossing, not replacements.
For patients managing gingivitis or recovering from periodontal therapy, prescription-strength antimicrobial rinses containing chlorhexidine may be recommended for short-term use. These are medical interventions for specific conditions, not daily maintenance products.
Tongue Cleaning: Often Overlooked, Always Important
Your tongue’s surface provides habitat for bacteria that contribute to bad breath and can recolonize teeth after cleaning. Use a tongue scraper or your toothbrush to gently clean your tongue daily, working from back to front. This simple step significantly improves oral freshness and reduces overall bacterial load.
Timing and Consistency
The biofilm lifecycle means consistency matters more than perfection. Missing a day of flossing allows biofilm to mature undisturbed. Missing several days allows calculus to begin forming. The goal is daily disruption—preventing biofilm from ever reaching maturity.
At Avra Dental, we help patients develop sustainable routines tailored to their specific needs. If you have orthodontic appliances, implants, or complex restorative work, your home care protocol needs to address those unique challenges. We provide personalized instruction because one-size-fits-all advice doesn’t account for individual oral architecture and risk factors.
Nutrition as Medicine: Foods That Remineralize and Protect
What you eat directly affects the chemical environment in your mouth—and therefore your susceptibility to decay and disease.
The Remineralization Equation
Tooth enamel exists in constant flux between demineralization (mineral loss) and remineralization (mineral redeposition). When you consume sugars or starches, bacteria metabolize them into acid, dropping oral pH and pulling minerals out of enamel. When pH returns to neutral, saliva—which is supersaturated with calcium and phosphate—deposits minerals back into enamel.
The balance between these processes determines whether enamel strengthens or weakens over time. Nutrition influences both sides of this equation.
Calcium and Phosphorus: The Building Blocks
Calcium-rich foods support remineralization by ensuring adequate mineral availability in saliva. Dairy products—milk, cheese, yogurt—are excellent sources. Cheese is particularly beneficial; it stimulates saliva production while providing calcium and raising oral pH, creating ideal conditions for remineralization.
For those who don’t consume dairy, alternatives include fortified plant milks, leafy greens (kale, collard greens, bok choy), almonds, and calcium-fortified foods. Phosphorus, found in eggs, fish, lean meats, and legumes, works synergistically with calcium in the remineralization process.
Vitamin D: The Absorption Catalyst
Without adequate vitamin D, your body cannot effectively absorb calcium—making even a calcium-rich diet less effective for dental health. Sources include fatty fish (salmon, mackerel), egg yolks, fortified foods, and sunlight exposure. For patients with documented vitamin D deficiency, supplementation may be necessary to support oral and systemic health.
Vitamin C and Gum Health
Vitamin C is essential for collagen synthesis—the structural protein that gives gum tissue its integrity. Deficiency leads to weakened, bleeding gums and impaired healing. Citrus fruits, berries, bell peppers, and cruciferous vegetables provide ample vitamin C. However, be mindful of timing: acidic fruits should be consumed as part of meals rather than sipped throughout the day, to limit enamel exposure to acid.

Crunchy Vegetables: Nature’s Toothbrush
Fibrous vegetables like carrots, celery, and apples require significant chewing, which stimulates saliva production. Saliva is your mouth’s natural defense system—it neutralizes acids, washes away food particles, and provides minerals for remineralization. These foods also have a mild abrasive effect that helps clean tooth surfaces mechanically.
Water: The Universal Protector
Water, especially fluoridated water, serves multiple protective functions. It dilutes acids, washes away food debris, and—in fluoridated communities—provides low-level, constant fluoride exposure that supports remineralization. In Ventura, our community water contains fluoride, making regular water consumption a simple preventative measure.
Replace sugary beverages with water whenever possible. Every sip of soda or juice creates an acid attack lasting 20-30 minutes. Frequent consumption means your teeth spend most of the day in an acidic, demineralizing environment.
Foods to Limit: The Acid and Sugar Problem
Sugary foods and beverages provide fuel for acid-producing bacteria. But frequency matters more than quantity. Sipping a sugary drink for hours creates continuous acid production. Consuming the same drink with a meal, followed by water, limits the duration of acid exposure.
Acidic foods and drinks—citrus, tomatoes, vinegar-based dressings, carbonated beverages—directly erode enamel through chemical action, independent of bacterial activity. This erosion is cumulative. If you consume acidic foods or drinks, do so with meals and rinse with water afterward. Avoid brushing immediately after acidic exposure; wait 30 minutes to allow saliva to neutralize pH and begin remineralization, as brushing during the acid-softened state can damage enamel.
Sticky foods like dried fruits, gummy candies, and caramels are particularly problematic because they adhere to teeth, prolonging exposure to sugars and acids.
Meal Timing and Snacking Patterns
Your teeth can handle occasional acid challenges—that’s what the remineralization process is designed for. What overwhelms this natural defense is constant challenge. Frequent snacking means your mouth never returns to neutral pH, preventing remineralization and keeping enamel in a perpetually weakened state.
Limiting eating occasions to defined meals and snacks, with water-only periods between, gives your saliva time to do its protective work. This pattern matters as much as what you eat.
At Avra Dental, we discuss nutrition not as a lecture but as a practical tool. Small, sustainable changes in eating patterns can significantly shift the balance toward remineralization and away from decay—especially for patients at high caries risk.
Preventative Care Across Life Stages: Why the First 1,000 Days Matter Most
Oral health needs evolve throughout life, requiring age-specific preventative strategies. But the most critical window—the one with lifelong implications—is early childhood.
The First 1,000 Days: Establishing Oral Immunity
The period from pregnancy through a child’s second birthday represents a unique opportunity to establish healthy oral microbiome patterns. During this window, the bacterial communities in a child’s mouth are being established. The species that colonize first have a competitive advantage, shaping the oral ecosystem for years to come.
Mothers with active, untreated dental disease can transmit high levels of cariogenic (cavity-causing) bacteria to their infants through saliva contact—sharing utensils, cleaning pacifiers with their mouth, or kissing. This early transmission increases the child’s cavity risk significantly.
Prenatal dental care isn’t just safe—it’s essential. Treating maternal gum disease and decay before birth reduces bacterial transmission and improves pregnancy outcomes. Periodontal disease has been linked to preterm birth and low birth weight, making dental care during pregnancy both preventative dentistry and prenatal care.
Once teeth begin erupting (typically around 6 months), they’re immediately susceptible to decay. Early childhood caries can develop rapidly, affecting not just baby teeth but also the developing permanent teeth beneath them. Establishing daily cleaning routines from the first tooth, limiting sugary drinks (especially in bottles), and scheduling a first dental visit by age one sets the foundation for lifelong oral health.
Pediatric Preventative Care: Building Healthy Habits
For children, preventative care focuses on three priorities: habit formation, physical protection, and early intervention.
We teach parents proper cleaning techniques for baby teeth and transitioning to independent brushing as motor skills develop. Fluoride varnish applications every six months provide enamel strengthening during the critical period when permanent teeth are erupting. Dental sealants applied to permanent molars as they come in (typically ages 6 and 12) prevent decay in the deep grooves that are difficult for children to clean effectively.
Early orthodontic evaluation—around age 7—allows us to identify developing alignment issues when interceptive treatment is most effective. Guiding jaw growth and creating space for permanent teeth during this developmental window can reduce or eliminate the need for extensive orthodontic treatment later.
At Avra Dental, we create positive dental experiences for children. Our goal is to build trust and comfort, establishing the dental office as a safe, welcoming environment rather than a source of fear. This early emotional foundation influences whether patients maintain regular preventative care throughout life.
Adolescents: Navigating Independence and Risk
Teenagers face unique challenges: increased autonomy over diet and hygiene, orthodontic treatment, sports participation, and social pressures. Our preventative approach for this age group emphasizes education and empowerment rather than parental enforcement.
We discuss how dietary choices—energy drinks, frequent snacking, acidic beverages—affect oral health. We address the specific hygiene challenges of orthodontic appliances. We strongly recommend custom athletic mouthguards for students involved in contact sports, as dental injuries are common and often preventable.
This is also the age to discuss the oral health consequences of tobacco use, vaping, and oral piercings—topics that require straightforward information without judgment.
Adults: Maintenance and Risk Management
For adults, preventative care shifts toward maintaining what you have and managing emerging risk factors. Stress-related grinding (bruxism) can cause significant tooth wear and fractures; custom night guards provide protection. Hormonal changes during pregnancy affect gum health, requiring adjusted cleaning schedules. Certain medications cause dry mouth, dramatically increasing decay risk and necessitating supplemental fluoride and saliva substitutes.
For patients with existing restorative work—fillings, crowns, implants—preventative care includes monitoring these restorations for signs of failure or secondary decay. Catching problems early often means simple repairs rather than complete replacement.
Seniors: Adapting to Changing Needs
Older adults face distinct challenges: medication-induced dry mouth, gum recession exposing vulnerable root surfaces, maintaining existing dental work, and managing the oral health impacts of systemic conditions like diabetes.
Root surfaces lack enamel’s protective layer, making them highly susceptible to decay. Prescription-strength fluoride toothpaste and more frequent professional cleanings help manage this risk. Dry mouth—a side effect of many common medications—reduces saliva’s protective functions, requiring proactive management through hydration, saliva substitutes, and meticulous home care.
For patients with partial dentures, bridges, or implants, cleaning techniques must adapt to address these prosthetics. We provide specific instructions because improper care can lead to failure of these often-costly restorations.
We also coordinate with medical providers when necessary, as conditions like diabetes, cardiovascular disease, and osteoporosis have bidirectional relationships with oral health. Managing one supports managing the other.
Personalization: The Common Thread
Across all life stages, effective preventative care is personalized. Generic advice doesn’t account for individual risk factors, existing conditions, or life circumstances. At Avra Dental in Ventura, we develop customized preventative protocols based on your specific situation—because prevention isn’t one-size-fits-all.
The True Cost of Prevention vs. Intervention
Let’s talk about money, because the financial case for preventative dental care is as compelling as the health case.
A routine preventative visit—examination, professional cleaning, necessary X-rays—typically costs $100-$300. This is the baseline investment in maintaining oral health.
Compare that to restorative procedures. A single filling ranges from $150-$400 depending on size and location. A root canal costs $700-$1,500 per tooth, and that doesn’t include the crown needed afterward, which adds another $800-$1,500. A dental implant to replace a lost tooth runs $3,000-$4,500.
The math is stark: two preventative visits per year cost less than a single filling. One year of preventative care costs less than one root canal. The financial advantage of prevention compounds over time.
Insurance Structures Reflect This Reality
Most dental insurance plans cover preventative services—exams, cleanings, X-rays—at 80-100%, often with no out-of-pocket cost. In contrast, major restorative procedures are typically covered at 50% or less, leaving significant patient responsibility.
Insurance companies structure benefits this way because they understand that preventative care reduces their long-term payouts. For patients with dental insurance, maximizing preventative benefits is financially prudent—you’re using coverage you’ve already paid for to avoid future expenses that will be largely your responsibility.
The Hidden Costs of Neglect
Beyond direct dental expenses, untreated dental problems carry hidden costs. Lost work time for emergency appointments. Reduced productivity when you’re in pain. Missed school for children. The psychological impact of dental anxiety or embarrassment about oral health.
The systemic health connections we discussed earlier also have financial implications. Uncontrolled periodontal disease complicating diabetes management. Oral infections requiring medical intervention. The potential cardiovascular risks associated with chronic oral inflammation. While these connections are complex and multifactorial, maintaining oral health as part of overall health management makes both medical and economic sense.
Protecting Previous Investments
For patients who have already undergone restorative or cosmetic dental work, preventative care protects that investment. Without proper maintenance, even well-executed dental work has a limited lifespan. Regular professional care and excellent home hygiene extend the longevity of fillings, crowns, implants, and veneers—delaying or preventing the need for costly replacements.
The Generational Advantage
For families, establishing preventative care as a norm creates generational benefits. Children who grow up with regular dental visits and strong home care habits typically experience fewer dental problems throughout life. This pattern of prevention—rather than crisis-driven dental care—reduces lifetime dental expenses while maintaining better oral health.
Accessibility and Payment Options
We recognize that even preventative care represents an expense. For patients without dental insurance, many practices (including Avra Dental) offer membership plans or payment options that make regular preventative care more accessible. Community health centers and dental schools also provide reduced-cost preventative services.
The key insight is this: preventative dental care is an investment with measurable, predictable returns. The minor, regular cost of prevention protects against the major, unpredictable cost of treatment. From a purely financial perspective—setting aside all health considerations—prevention is the economically rational choice.
Advanced Diagnostic Technology: Catching Problems at the Cellular Level
Modern preventative dentistry has been transformed by diagnostic technologies that detect disease earlier, with greater precision, than ever before possible.
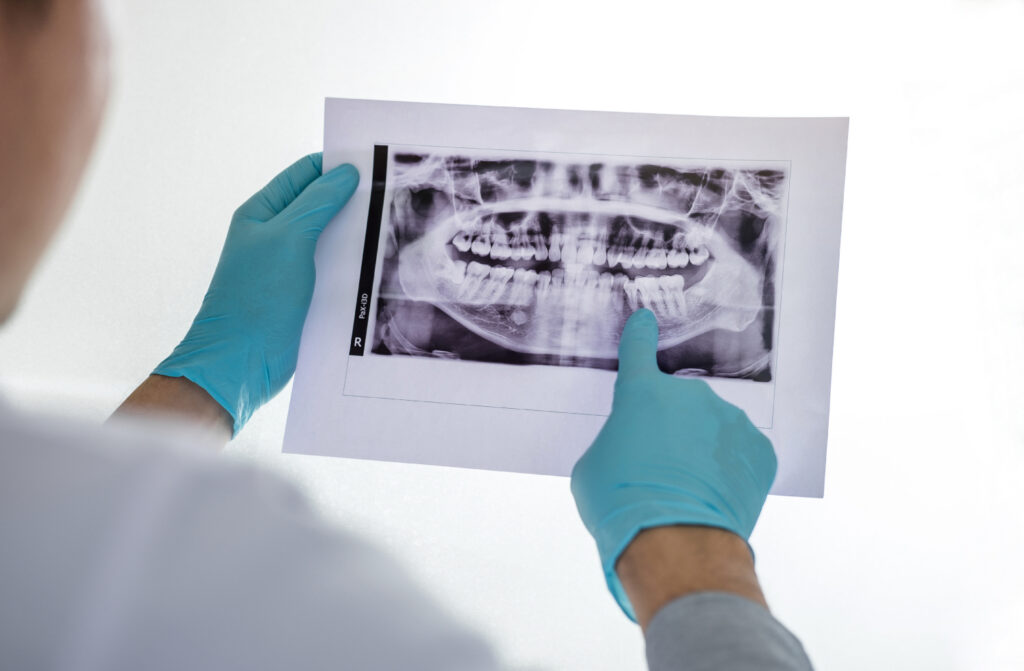
Digital Radiography: Seeing Beyond the Surface
Digital X-rays represent a fundamental improvement over traditional film. They use up to 90% less radiation while producing higher-resolution images that can be enhanced, magnified, and analyzed with diagnostic software.
This technology allows us to detect interproximal decay (between teeth) at very early stages—often before it’s clinically visible. We can measure bone levels with precision, tracking subtle changes over time that indicate active periodontal disease. We can identify developing abscesses, impacted teeth, root fractures, and pathology that would be invisible during clinical examination alone.
The ability to compare images side-by-side over the years reveals patterns. A small area of demineralization that hasn’t progressed might indicate successful remineralization efforts. Gradual bone loss around a specific tooth alerts us to localized periodontal issues requiring targeted intervention.
At Avra Dental, we use digital radiography as a standard diagnostic tool, providing detailed visual information while minimizing radiation exposure—a combination that wasn’t possible with conventional film.
Intraoral Cameras: Shared Visual Understanding
Intraoral cameras are small, pen-sized devices that capture highly detailed images of individual teeth and gum tissue. These images display immediately on a monitor, allowing patients to see exactly what we’re seeing.
This technology transforms the patient experience. Instead of describing a problem verbally, we can show you the hairline crack in your molar, the margin gap around an old filling, or the inflammation in your gum tissue. This shared visual understanding improves communication and helps patients make informed decisions about recommended treatments.
From a diagnostic standpoint, intraoral cameras allow documentation of conditions over time. We can track whether a suspicious area is changing, monitor healing after treatment, and identify problems in their earliest stages.
Laser Cavity Detection: Identifying Demineralization Before Cavitation
Laser fluorescence technology can detect changes in tooth structure at the molecular level—identifying areas of demineralization before they become cavities. The device measures the fluorescence of tooth structure; decayed or demineralized areas fluoresce differently than healthy enamel.
This early detection creates a treatment option that doesn’t exist with traditional diagnostic methods: remineralization therapy. When we identify demineralization before cavitation, we can attempt to reverse the process through intensive fluoride therapy, dietary modification, and improved biofilm management—potentially avoiding the need for restoration entirely.
This is minimally invasive dentistry at its core: intervening at the earliest possible stage with the least invasive treatment.
Extraoral Suction Systems: Infection Control as Prevention
At Avra Dental, we utilize an Extraoral Dental Suction System—a technology that captures aerosols and airborne particles generated during dental procedures. While this is primarily an infection control measure, it’s also a preventative technology, protecting both patients and staff from exposure to pathogens.
In the post-pandemic era, infection control has taken on heightened importance. Advanced safety measures like extraoral suction demonstrate our commitment to creating the safest possible environment for dental care.
The Philosophy Behind the Technology
Technology alone doesn’t create better outcomes—it’s how we use it. At our Ventura dental office, advanced diagnostic tools serve a specific philosophy: detect problems at their earliest, most treatable stages, and intervene with the least invasive approach that will effectively manage the condition.
This approach preserves natural tooth structure, reduces patient discomfort, and often provides more conservative treatment options than would be possible if problems progressed to the point of symptoms. It’s prevention through precision—using technology to catch disease before it causes damage.
What To Do Next: Your Personalized Prevention Plan Starts Here
Preventative dental care isn’t passive—it requires partnership. You bring consistent home care and health-conscious choices. We bring expertise, technology, and early intervention when problems develop.
If you haven’t had a comprehensive dental examination in the past six months, now is the time. At Avra Dental in Ventura, we’ll assess your current oral health status, identify any areas of concern, and develop a personalized preventative care plan tailored to your specific needs and risk factors.
We’re not just checking for cavities. We’re evaluating your periodontal health, screening for oral cancer, assessing your bite and jaw function, and looking for early signs of problems that haven’t yet caused symptoms. We’re using advanced diagnostic technology to see beyond what’s visible on the surface.
For new patients, we’re offering a comprehensive new patient special: examination, professional cleaning, and digital X-rays for $220—a significant value for the foundation of your preventative care.
For families, we provide care for all ages, from pediatric dentistry that makes children comfortable and establishes healthy habits, to adult preventative and restorative care, to specialized approaches for seniors managing complex dental needs.
If you’re experiencing any concerning symptoms—tooth sensitivity, bleeding gums, persistent bad breath, pain, or changes in your bite—don’t wait for your next scheduled visit. These are early warning signs that warrant prompt evaluation. We offer same-day emergency appointments because we know that dental problems don’t follow convenient schedules.
Ready to take control of your oral health?
Call Avra Dental to schedule your comprehensive preventative care appointment. We’re located at 1708 S Victoria Ave B in Ventura’s Montalvo Square Shopping Center—convenient, accessible, and equipped with state-of-the-art technology to provide the highest level of preventative care.
Your future smile starts with the decisions you make today. Let’s build your personalized prevention protocol together.

