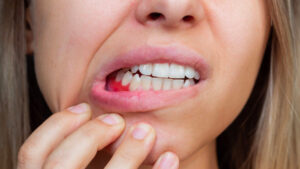
Gum disease affects nearly half of American adults over 30, according to the CDC. The most concerning part? Many people don’t realize they have it until significant damage has already occurred. If you’ve noticed blood on your toothbrush, experienced persistent bad breath, or felt unusual sensitivity in your gums, your mouth may be sending you an urgent message.
The good news: When caught early, gum disease (gingivitis) is completely reversible. The key is recognizing the warning signs before inflammation progresses to periodontitis—a condition that can lead to tooth loss, bone deterioration, and systemic health complications.
This guide will help you identify the seven early indicators of gum disease, explain what’s happening beneath the surface, and show you exactly when to seek professional care.
Why Early Detection Matters More Than You Think
Gum disease doesn’t announce itself with dramatic pain. It whispers through subtle symptoms that are easy to dismiss as “normal” or temporary.
Here’s what makes early detection critical:
When gum disease is in its initial stage (gingivitis), the inflammation affects only the gum tissue. At this point, professional cleaning combined with improved home care can completely reverse the condition. There’s no permanent damage.
But when gingivitis advances to periodontitis, the infection begins destroying the bone and connective tissue that hold your teeth in place. This damage is irreversible. Treatment can stop progression, but it cannot regenerate what’s been lost without surgical intervention.
The financial stakes are significant too. A routine cleaning and exam at Avra Dental costs far less than the deep cleanings, gum grafting, or implant procedures required to treat advanced periodontal disease.
Beyond your mouth, research from the American Academy of Periodontology shows connections between untreated gum disease and increased risk of heart disease, diabetes complications, and respiratory infections. Your gums are not isolated—they’re connected to your overall health.
The message is clear: The symptoms you’re experiencing today deserve attention now, not later.
Visual Indicators Your Gums Are in Trouble
Healthy gums have a distinct appearance: firm, pale pink, and fitting snugly around each tooth like a protective collar. Any deviation from this baseline deserves investigation.
Bleeding During Brushing or Flossing
If you see pink or red in the sink after brushing, your gums are inflamed.
This is not normal, despite how common it is. Healthy gum tissue should not bleed from the gentle pressure of a toothbrush or floss. The bleeding occurs because plaque bacteria have colonized along your gumline, triggering your immune system to flood the area with blood vessels. These engorged, fragile vessels rupture easily.
This is typically the first visible sign of gingivitis. The inflammation is your body’s alarm system—it’s calling for help to fight the bacterial invasion.
What to watch for:
- Blood on your toothbrush or floss
- Pink-tinged saliva when you spit
- Bleeding that occurs consistently, not just once
What it means: Plaque buildup has been present long enough to cause a sustained inflammatory response. The good news? This stage is still reversible with professional cleaning and improved daily hygiene.

Swollen, Red, or Puffy Gums
Gum tissue should lie flat against your teeth. When it appears puffy, red, or swollen—especially between teeth—inflammation has progressed beyond the initial stage.
The color change tells the story. Healthy gums are pale pink. Inflamed gums turn darker red or even purplish because of increased blood flow to the infected area. The swelling occurs as your immune system sends fluid and white blood cells to combat bacteria.
You might notice:
- Gums that look shiny instead of matte
- Tissue that feels spongy or tender when touched
- Gum tissue that extends higher up the tooth than it used to
- Discomfort when chewing or brushing
Why this matters: Swelling indicates the infection has established itself. The longer inflammation persists, the more likely it is to damage the periodontal ligament—the connective tissue anchoring your teeth to bone.
Gum Recession (Teeth Looking Longer)
Have your teeth started to look longer? That’s not growth—it’s exposure.
Gum recession occurs when inflamed tissue pulls away from the tooth, exposing the root surface. This happens gradually, which is why many people don’t notice until several millimeters of root are visible.
What causes this?
- Chronic inflammation is destroying gum attachment
- Aggressive brushing with hard-bristle brushes
- Genetic predisposition to thin gum tissue
- Tobacco use, which restricts blood flow to the gums
Signs of recession include:
- Visible yellow or darker areas near the gumline (that’s the root surface, not enamel)
- Notches or grooves where the gum meets the tooth
- Increased sensitivity to cold, heat, or sweet foods
- Teeth appearing longer or more spaced out than before
Recession is particularly concerning because once gum tissue recedes, it rarely grows back on its own. Early intervention can prevent further loss, but advanced cases may require gum grafting procedures to restore coverage and protect exposed roots.
Sensory Symptoms You Shouldn’t Ignore
This is where most online resources fall short. They list the obvious visual signs but overlook the subjective sensory experiences that often appear first. These symptoms validate what you’re feeling—and they’re legitimate warning signs.
Persistent Bad Breath or Metallic Taste
If brushing, flossing, and mouthwash don’t eliminate your bad breath, the problem is deeper than surface bacteria.
Chronic halitosis (persistent bad breath) is caused by volatile sulfur compounds—gases produced by anaerobic bacteria thriving in the oxygen-poor environment of gum pockets. As gum disease progresses, these pockets deepen, creating ideal conditions for odor-producing bacteria.
You might also notice:
- A constant metallic or sour taste, even after brushing
- Bad breath that returns within an hour of cleaning your teeth
- Others commenting on your breath (often the first external indicator)
- A white or yellow coating on your tongue that returns quickly after scraping
Why mouthwash isn’t enough: Antiseptic rinses temporarily mask odor but don’t address the bacterial colonies living beneath the gumline. Only professional cleaning can remove the calcified tartar harboring these bacteria.
Increased Tooth Sensitivity to Temperature
Does cold water make you wince? Do hot beverages cause sharp discomfort?
While tooth sensitivity can have multiple causes (enamel erosion, cavities, cracked teeth), gum recession from periodontal disease is a primary culprit. When gums recede, they expose the tooth root, which lacks the protective enamel layer covering the crown.
This exposes microscopic tubules that lead directly to the tooth’s nerve center. Temperature changes, acidic foods, and even cold air can trigger sharp, shooting pain.

Key distinctions:
- Gum disease-related sensitivity: Affects multiple teeth, especially along the gumline; worsens over time
- Cavity-related sensitivity: Usually localized to one tooth; triggered by sugar and pressure
- Enamel erosion: Affects biting surfaces; caused by acidic foods or aggressive brushing
If your sensitivity is widespread and concentrated near the gumline, gum recession from inflammation is the likely cause.
Itchy or Uncomfortable Gum Sensation
This is the symptom most people hesitate to mention because it sounds unusual. But it’s remarkably common in early gum disease.
Patients describe it as:
- A persistent urge to press or massage the gums
- An uncomfortable “crawling” sensation along the gumline
- Gums that feel tight or irritated
- Relief when pressing on the gums with a finger or tongue
What causes gum itching? Inflammation triggers the release of histamines—the same compounds responsible for itching in allergic reactions. As your immune system responds to bacterial toxins, histamine release can create that characteristic itchy sensation.
This symptom often appears before visible swelling or bleeding, making it an early warning sign that’s easy to dismiss. If you’re experiencing gum itching along with any other symptom on this list, schedule an assessment.
Physical Signs of Advancing Gum Disease
Loose or Shifting Teeth
Adult teeth should never feel loose. If they do, significant bone loss has likely occurred.
By the time teeth become mobile, gum disease has progressed to moderate or advanced periodontitis. The infection has destroyed enough of the supporting bone and periodontal ligament that teeth can no longer maintain their stable position.
Warning signs include:
- Teeth that wiggle when you press on them with your tongue or finger
- Changes in how your teeth fit together when you bite
- Gaps are developing between teeth that were previously tight
- Difficulty chewing tough or sticky foods
- Pain when biting down
This is a dental emergency. Loose teeth indicate that the structural support system is compromised. Without immediate intervention—often involving deep cleaning (scaling and root planing), antibiotics, or surgical treatment—tooth loss becomes inevitable.
At Avra Dental, we use advanced diagnostic technology to assess bone levels and create personalized treatment plans to stabilize teeth and prevent further deterioration.
What Causes These Warning Signs? Understanding the Inflammation Process
Gum disease doesn’t happen overnight. It’s the result of a specific biological process.
Here’s the sequence:
1. Plaque Formation: Within hours of eating, bacteria colonize your teeth, forming a sticky biofilm called plaque. This film is constantly forming and must be mechanically removed through brushing and flossing.
2. Calcification: If plaque isn’t removed within 24-48 hours, minerals in your saliva harden it into tartar (calculus). Tartar cannot be removed with a toothbrush—only professional instruments can eliminate it.
3. Immune Response: Bacteria in plaque and tartar release toxins that irritate gum tissue. Your immune system responds by sending white blood cells and increasing blood flow to the area, causing redness, swelling, and bleeding.
4. Tissue Destruction: If inflammation persists, your immune system begins breaking down the connective tissue and bone supporting your teeth. This is your body’s attempt to create distance between healthy tissue and the bacterial threat—but it backfires, destroying the structures you need to keep your teeth.
Risk factors that accelerate this process:
- Smoking: Reduces blood flow to gums, impairing healing and immune response
- Diabetes: High blood sugar feeds bacteria and impairs infection-fighting ability
- Genetics: Some people have naturally aggressive immune responses that cause more tissue damage
- Stress: Elevates cortisol, which suppresses immune function
- Medications: Certain drugs (antihistamines, antidepressants) cause dry mouth, reducing saliva’s protective effects
Understanding this process explains why early intervention is so powerful. When you address inflammation at the gingivitis stage, you stop the cascade before permanent damage occurs.
Your Next Steps: From Home Care to Professional Assessment
If you’ve identified one or more warning signs in yourself, here’s your action plan:
Immediate Home Care Improvements
While home care alone won’t reverse established gum disease, these steps prevent further progression:
- Brush for two full minutes, twice daily, using a soft-bristled brush and fluoride toothpaste. Focus on the gumline, where plaque accumulates.
- Floss once daily using proper technique: curve the floss around each tooth in a C-shape and gently slide beneath the gumline.
- Use an antiseptic mouthwash to reduce bacterial load (this is supplementary, not a replacement for brushing and flossing).
- Stay hydrated to maintain saliva production, which naturally cleanses your mouth.
- Avoid tobacco in all forms—it’s one of the most significant risk factors for gum disease progression.
When to Schedule a Professional Assessment
You should contact Avra Dental if you’re experiencing:
- Bleeding gums that persist for more than a week despite improved brushing
- Visible swelling, redness, or recession
- Persistent bad breath that doesn’t resolve with oral hygiene
- Any tooth sensitivity or mobility
- Gum discomfort, itching, or pain
What to expect during your gum health assessment:
Dr. Tariq Jabaiti and our team will perform a comprehensive periodontal evaluation, including:
- Probing depths: Measuring the space between your gums and teeth to assess pocket depth (healthy gums have pockets of 1-3mm)
- Bleeding on probing: Checking for inflammation by gently probing the gumline
- Digital X-rays: Evaluating bone levels to detect any loss
- Visual examination: Assessing gum color, texture, and attachment
Based on findings, we’ll create a personalized treatment plan. For early-stage gingivitis, this typically involves professional cleaning and education on proper home care techniques. For more advanced cases, we may recommend scaling and root planing to remove bacteria from beneath the gumline.
Our commitment: We use state-of-the-art technology and advanced techniques to provide precise, comfortable care in a welcoming environment. You’re not just another patient—you’re part of our dental family, and we’re here to guide and support you through every step of treatment.
Frequently Asked Questions About Gum Disease Warning Signs
What are the very first signs of gum disease?
The earliest signs are often subtle: occasional bleeding when brushing, slight gum tenderness, or mild bad breath that returns quickly after brushing. Many people also notice a change in gum color from pale pink to slightly darker red. These symptoms indicate gingivitis—the only reversible stage of gum disease.
Can gum disease go away on its own without treatment?
No. Gum disease is caused by bacterial infection and your body’s inflammatory response. Without removing the source (plaque and tartar), the infection will persist and worsen. However, early-stage gingivitis can be reversed with professional cleaning combined with improved home care. Advanced periodontitis cannot be reversed, but can be managed to prevent further damage.
How quickly does gum disease progress from gingivitis to periodontitis?
Progression varies significantly based on individual factors like genetics, oral hygiene, smoking, and overall health. In some people, gingivitis can persist for years without advancing. In others—particularly smokers or those with diabetes—progression to periodontitis can occur within months. This is why regular dental assessments every six months are crucial for monitoring gum health.
Is bleeding when I floss normal if I don’t floss regularly?
Bleeding indicates inflammation, which means gum disease is present—even if it’s mild. When you resume flossing after a break, you’re disturbing inflamed tissue, which causes bleeding. With consistent daily flossing and proper technique, bleeding should resolve within 1-2 weeks as inflammation decreases. If it persists beyond two weeks, schedule a professional cleaning.
Can gum disease affect my overall health?
Yes. Research shows connections between periodontal disease and several systemic conditions. The inflammation and bacteria from gum infections can enter your bloodstream, potentially contributing to cardiovascular disease, complicating diabetes management, increasing respiratory infection risk, and even affecting pregnancy outcomes. The American Academy of Periodontology emphasizes that oral health is inseparable from overall health.
How often should I see a dentist if I’m at risk for gum disease?
For most adults with good oral health, professional cleanings every six months are sufficient. However, if you have a history of gum disease, diabetes, smoke, or have genetic risk factors, Dr. Jabaiti may recommend cleanings every 3-4 months. More frequent visits allow us to monitor gum health closely and remove bacterial buildup before it causes damage.
What’s the difference between gingivitis and periodontitis?
Gingivitis is inflammation of the gum tissue only. It causes redness, swelling, and bleeding, but doesn’t affect the bone or connective tissue supporting teeth. It’s completely reversible.
Periodontitis is advanced gum disease where inflammation has destroyed the periodontal ligament and bone. This creates deep pockets between teeth and gums, causes gum recession, and can lead to tooth mobility and loss. Periodontitis is not reversible, though treatment can halt progression.
Don’t Wait for Pain—Gum Disease Progresses Silently
Here’s what you need to remember: Gum disease rarely causes pain in its early stages. By the time you experience discomfort, significant damage may have already occurred. The warning signs we’ve discussed—bleeding, swelling, recession, sensitivity, bad breath, itching, and mobility—are your early alert system.
Taking action now means:
- Reversing gingivitis before it becomes periodontitis
- Avoiding costly restorative procedures like gum grafting or implants
- Protecting not just your oral health, but your overall wellness
- Maintaining your natural teeth for life
At Avra Dental, we believe in prevention-focused care that addresses problems before they escalate. Our Ventura dental office combines state-of-the-art diagnostic technology with compassionate, personalized treatment in a comfortable and welcoming environment.
Schedule Your Gum Health Assessment Today
If you’ve recognized any of these warning signs, we’re here to help.
Dr. Tariq Jabaiti, a USC dental faculty member specializing in preventive and restorative dentistry, leads our experienced team in providing thorough dental services that address every aspect of your oral health. We accept most major insurance plans and offer flexible scheduling to fit your busy life.
New patients can take advantage of our special offer:
- Comprehensive exam, professional cleaning, and digital X-rays for $220
Don’t let uncertainty keep you from getting the care you need. Whether you’re experiencing mild symptoms or significant concerns, we’re here to guide and support you with prompt, expert care.
📞 Call Avra Dental today or visit us at 1708 S Victoria Ave B, Ventura, CA 93003 (Montalvo Square Shopping Center) to schedule your gum health assessment. Your smile—and your overall health—will thank you.